Cholecystectomy:
The goal of cholecystectomy is to remove the gallbladder cyst in most cases due to the presence of gallstones in the gallbladder that lead to symptoms such as: Pains Feeling uncomfortable Bile tract obstruction or gallbladder cyst infection.
Gallstones are the most common reason for gallbladder removal.
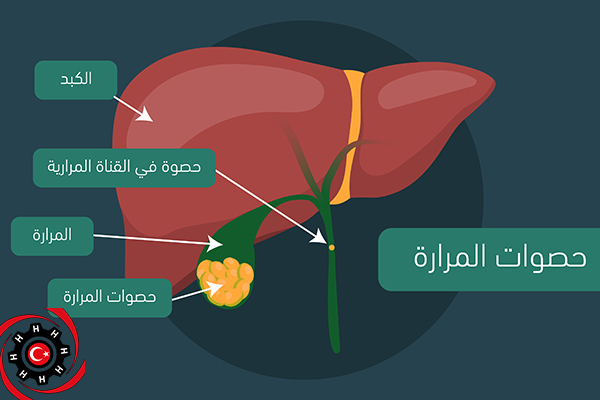
The gallbladder cyst is a storehouse of bile acids in the digestive system, which flow into the bile ducts, liver or intestines in order to contribute to the absorption of fats from food into the blood.
Gallstones are formed due to the accumulation of sediment, which is often composed of cholesterol, calcium and pigment (pigment) in the gallbladder sac.
In most cases, stones in the gallbladder do not cause any symptoms, but the stones that block the entrance to the gallbladder sac or the bile duct cause severe pain, jaundice, and the accumulation of bacteria, which may cause acute inflammation of the gallbladder sac.
Cholecystitis is treated with antibiotics and surgery.
Today, most of the gallbladder removal operations in the world are done using endoscopy. This technique includes making three small incisions in the abdomen, inserting a long and thin device at the end of which there is a very small camera, through which the surgeon can view the abdominal cavity through the screen and remove the gall bladder from its place using a device suitable.
Another possibility to remove the gallbladder cyst is through an open surgery, where the abdomen is opened by making a larger incision, and then the gallbladder cyst is removed.
Open surgery is more preferable if there is a suspicion of cancer.
Preparing for the operation:
The patient is given appropriate antibiotics before the surgery in order to reduce local inflammation and thus reduce the possibility of infection after the operation.
The patient needs to have the following blood tests:
Complete blood count, blood chemistry, coagulation tests, urine examination, liver and kidney function tests, and bilirubin level in the blood.
Imaging tests that the patient needs to do are, an empty stomach image (in order to rule out perforation of the gallbladder), examination of the biliary tract using ultrasound, scanning of the biliary tract using radioisotopes and sometimes computed tomography (CT).
The patient undergoes the surgery under general anesthesia. The doctor should be consulted regarding the medications that the patient should stop taking for a few days before the operation, and he should fast for at least 8 hours before the operation.
process:
The general surgeon performs the gallbladder cyst removal.
In the operation that is done using the laparoscope, the abdominal area is cleansed, and 4 small incisions (about 1-3 cm) are made in the abdominal area close to the navel, and in additional places around the gallbladder sac, through these incisions the arms of the telescope are inserted.
Later, the abdomen is expanded by inserting gas through the holes, in order to improve the range of vision of the internal organs in the abdomen by endoscope, as what is happening in the abdomen is watched on a TV screen.
In the open surgery, one longer incision is made in the right upper abdominal wall to reach the abdominal cavity.
After the surgeon explores the abdominal cavity, locates the gallbladder cyst and separates it from the blood supply and from the bile duct.
After that, the gallbladder cyst is removed and removed through one of the openings.
During the operation, the bile ducts are examined with a contrast material (Contrast) in order to ensure that there are no stones that would block these bile ducts.
In the event that additional stones are detected, they are extracted during the operation.
Upon completion of the surgery, the abdominal wall and incisions are sutured and bandages are placed on them.
The surgery takes one to two hours.
Operation risks:
General risks of surgery:
Surgical incision infection – often superficial and treated topically.
But in some rare cases, the matter may develop into a more serious infection in the subcutaneous layers, and the infection may reach the abdominal wall and cavity.
Sometimes the doctor may have to open the incision again in order to get rid of bacteria residues.
Bleeding – primarily in the surgical area following local tissue damage.
Bleeding may occur immediately after the operation within the next 24 hours and in rare cases weeks after the operation.
In cases where the bleeding is significant, it must be stopped by surgical means (another operation is to electrically burn the bleeding site or tie off the blood vessels causing the bleeding).
Scar The uniformity of the scar from the surgical incision to healing is related to the type of suture and genetics.
There is no way to predict how the scar will heal after the operation, but since the incisions that the surgeon makes in the laparoscopic surgery are very small, it is expected that very small scars will remain.
The risks of anesthesia The phenomena are often caused by hypersensitivity to the anesthetic drugs (allergic response).
Epidural anesthesia often causes temporary mild muscle spasms or a headache.
In very rare cases, a serious reaction may occur that leads to a drop in blood pressure (anaphylactic shock).
Special risks:
Injury to the intestines or liver due to being in close proximity to the gallbladder sac is rare.
Injury to the bile duct may lead to leakage of the contents of the gallbladder into the abdominal cavity, which may cause chemical inflammation of the peritoneum.
Injury to the diaphragm due to being in close proximity to the surgical area.
Allergy to contrast material may lead to kidney failure.
Post-operative treatment:
After the operation to remove the gallbladder cyst using a laparoscope, the patient lies for 24-48 hours in the hospital in order to monitor his medical condition.
The electrode is removed after about a week.
Thus, it causes less pain and the patient stays for a shorter period in the hospital.
Recovery after open surgery takes longer.
The patient can take painkillers if he feels pain.
In the following cases, the patient should go directly to the doctor:
Feeling of pain that does not go away even with the use of painkillers, high fever, inability to urinate, shortness of breath, strong bleeding or purulent secretions from the surgical incision.

Leave a Reply